Oct 24, 2018 Politics
From the Metro archives: Fighting for Zac
This story originally appeared in the November 2010 edition of Metro.
A father determined to find out why his son died from meningitis had to battle an obdurate hospital bureaucracy and a closed shop of doctors.
On July 8 last year, Auckland City Hospital, like every other, was by its own admission “run off its feet” with swine flu. Front page headlines in that morning’s New Zealand Herald told how medical centres were struggling to cope with a rising flood of cases, with patient numbers up 40 per cent. The number of swine-flu hospitalisations had peaked the day before, at 38.
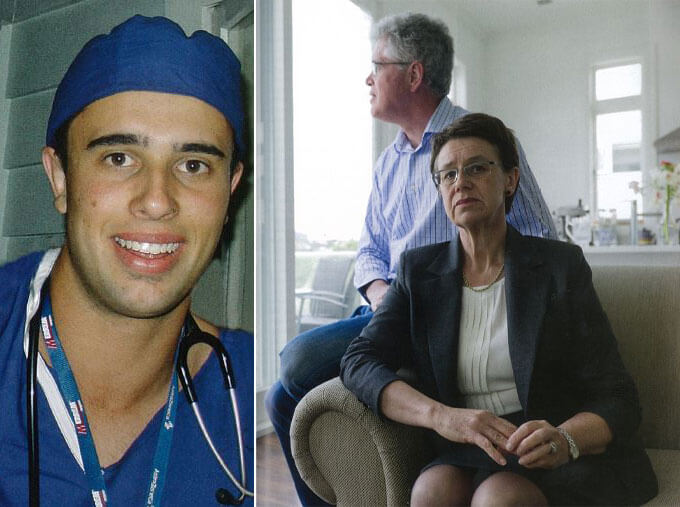
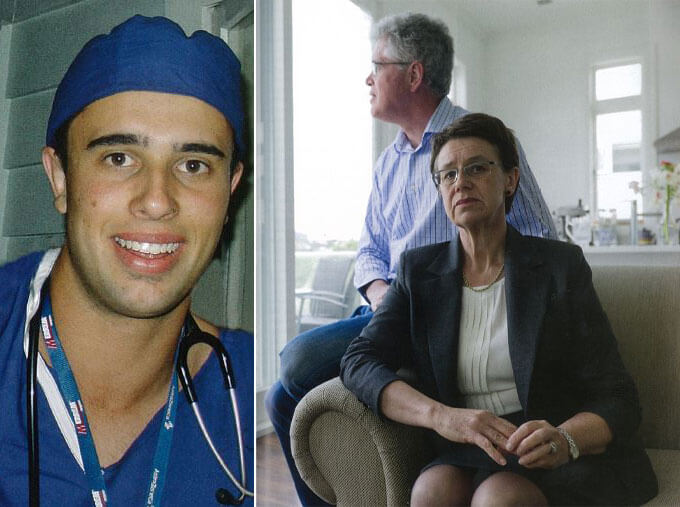
Fourth-year medical student Zac Gravatt, 22, probably didn’t read the story when he woke at 4am feeling as grotty as hell. By the time he saw the local doctor around 11am, swine flu was the prime suspect. Just the week before, he told the GP, he’d been in contact with swine-flu patients on the wards. The GP didn’t hesitate, ordering his immediate transfer by ambulance to Auckland City Hospital.
Mask-wearing paramedics found a constellation of worrying signs — a racing pulse, high fever (nudging 40 degrees), rapid breathing, and lowish blood pressure. By 1.43pm, Zac was in triage at the emergency department, where a nurse assigned him “category 3” — a designation which under emergency department guidelines means treatment should begin within a maximum of 3o minutes.
But treatment did not begin in 30 minutes, 60 minutes or 120 minutes. From 2.30pm to4pm, when the unit was at 80 per cent capacity, staff didn’t even record his vital signs, nor did they give pain relief or fluids to this critically ill young man. It was “care” that even the health board’s own independent expert describes as unacceptable.
By 4.30pm, when antibiotics were finally given, Zac had less than three hours to live. And even then, the country’s premier centre of medical excellence had failed to diagnose the meningococcal septicaemia that was rapidly killing him.
“The only window of opportunity he had,” says Lance Gravatt, “was when he first came in, and he was not even given a chance of life. No one can say with certainty what the outcome would have been but he should have been given the chance. You know, to put him in a room and just leave him there for a few hours… he deserved better than that. New Zealand deserves better than that.”
The Gravatts returned to Auckland City Hospital the day after Zac’s death, to thank those responsible for his care. They had no idea then how little they had to be thankful for.
They also needed to fill in the gaps for themselves because during his critical hours in the emergency department, Zac was alone. Lance, Jenny and daughter Maddy were in Wellington for a Supreme Court case that Lance’s company was involved with. They flew back as soon as Zac told them he was in hospital, but they arrived less than two hours before he died.
Jenny, a resource management planner, read the notes first, and while her first thought was that “the timing didn’t gel”, she found it difficult to piece the story together. Lance couldn’t face the task straight away and it was not until the Christmas holidays that he finally read the records.
For Lance, the chief executive of an international pharmaceutical company and with a PhD in organic chemistry, the notes were deeply troubling. “The first thing that struck me was the lab report of his blood tests. They said he had low platelets and low white cells which are present in the setting of sepsis — consistent with infection. And I thought, ‘Well, no one ever said that.'”
Even the consultant who saw Zac at 5.30pm, when Zac had only 90 minutes left to live and was already coming out in the telltale meningococcal rash, told the Gravatts he still thought their son had an “influenza-like virus”. He was transferring him to critical care, he said, to help him with his breathing.
But Lance says Ministry of Health guidelines say flu-like illness is defined as a history of fever, chills and sweating plus a cough or sore throat. Zac had no cough and no sore throat, so statistically, at the time he arrived at Auckland City Hospital, the likelihood of his having swine flu was less than five per cent. His symptoms — high fever, fast heart rate, low blood pressure and rapid breathing — were, Lance believes, “screaming infection”.
“I thought to myself, ‘Right Lance, you’ve found something that concerns you, let’s lay it all out systematically and anything I don’t understand, I’ll just Google it and research it.’ That’s when I found out triage category 3 means he should be seen in a maximum 30 minutes — and he wasn’t seen for more than two hours. Then I find that low blood pressure is a sign of organ failure with sepsis. So you start laying out these concerns one after another after another and it just got worse and worse and your heart just sank more and more. In the end, you get this sense of, ‘What did they do right?”
The Gravatts thought carefully about what to do next. “I’ve seen it so many times before on TV, of grieving, distraught parents with a kind of conspiracy theory, making fools of themselves or embarrassing themselves in front of the nation with their grief, when their concerns are not factually based, or a bit irrational — and we said, ‘We don’t want to be one of them.”
So Lance documented his findings and sent them off to the Health and Disability Commissioner and the coroner and emailed Auckland District Health Board chief executive Garry Smith.
Smith never replied — or even acknowledged receipt of the email — a discourtesy which so annoyed Lance that he called the Herald. The newspaper’s inquiries prompted a call from the board’s chief medical officer, David Sage, who said he’d been unaware of the family’s concerns, and invited them in to go over the notes.
“I said I didn’t buy that this was the first they’d heard of our concerns — I’d emailed Garry Smith and I thought, ‘OK you guys, someone somewhere in your good ship lollipop has known about it.” Sage told the Herald he was “absolutely confident” Zac had received the best possible care.
“I would like to reassure the public that when a patient comes into our care, they are in an expert centre with vast experience in the early diagnosis of [swine] flu and meningococcal disease.” The comment further angered the Gravatts, who by this time had obtained a report for the coroner by a hospital intensivist who said that, in his opinion, Zac had “overwhelming meningococcal sepsis at the time of presentation to hospital”.
His death may have been inevitable even with earlier antibiotic therapy and early intensive care.
For the Gravatts, there was only one problem with that — the word “may”. The chance, the lost chance, that Zac might have been saved. Alerted to the possibility Zac’s death could be classified as an ACC treatment injury, Lance filled out an application form — not to get the money, but for an independent report on his son’s care from ACC’s medical expert. He then discovered a doctor had to sign the form, but Zac’s hospital consultant had died of a heart attack, their GP had retired and moved away and he knew of no other doctor who’d known Zac.
“I asked if ACC could suggest any doctors and they said, ‘No, you’ll have to find yourself one.’ Then I phoned the health commissioner and the coroner and I remember crying and crying. I said, ‘Are you telling me I’ve got to walk around Auckland, door-knocking with my dead son’s medical records tucked under my arm to see if I can find someone who will read them and then, if they’re of a mind to, sign them?’
“They said, ‘That’s right.”‘
He finally found a GP who not only signed the form, but also endorsed his concerns about the shortcomings in Zac’s care. Lance then asked for a copy of the hospital’s own morbidity and mortality review of the case — the record of a meeting held every two months in which medical staff review adverse events — and discovered there hadn’t been one. “We were absolutely gobsmacked.”
He says the DHB’s medico-legal counsel told him many people died every day at Auckland City Hospital and “you can’t investigate them all”.
“I said, ‘They won’t all be young, fit, healthy men like Zac who were not expected to die and of whom your own notes set out that you got the diagnosis wrong.’ “He said, ‘Look, Zac had an awful disease and he would have died anyway.’ I said, ‘How do you know that when you haven’t investigated?’ There was no response to that.”
That, too, was his concern with Sage’s public reassurances. “He told the public Zac got the best of care. But he had no basis on which to say it — and it was such a put-down to us.”
“I felt at the time that I was under immense pressure to either drop my complaint and keep my job or press on with the complaint and run the risk of losing my job.” He said he never put his job title on emails to the board and often signed correspondence “Zac’s dad”. The company’s phone interview over the complaint reduced him to tears. “In the end, I thought, ‘If I’ve got to lose my job, I’ll lose my job. I’ve got to stand up for my son.’ That’s what I kept saying to them — it’s every dad’s right to stand up for his son.” He later received an email telling him the company would not take the matter further.
When the DHB told the Gravatts it had commissioned an independent report from Middlemore consultant physician Roger Reynolds, they were initially un-convinced. “Their lawyer said it would show Zac received the best of care,” Lance said. “At that point we really felt this was not independent at all — how can he possibly know the outcome of a report that’s not yet been written of a review that’s not been done?”
His confidence eroded, Lance sought his own independent expert, but found instead a medical closed shop. “Everyone I spoke to offered condolences but said they were either too busy or not the right people.”
He and his lawyer approached 15 to 20 specialists nationally before finding a doctor at a neighbouring Auckland hospital who agreed to review the notes. “He phoned back and said, ‘Lance, I was hoping when I opened this envelope I’d go through Zac’s records and be able to reassure you that the best that could have been done had been done and allayed your concerns. But I can’t. All the concerns you’ve raised are spot on.’ “He said as a doctor this is just the ‘worst, worst-case scenario: that you’ve had a young person die is bad, that it may have been preventable is worse, that makes it more than worse, and worse again, they were a colleague..”.
But he, too, declined to write a formal report, saying that because he worked in Auckland, it was “too close to home”.
“I started to get this feeling of this huge machine we’re up against here. Fortress Medicine has raised the drawbridge and turned off the lights and you can try to batter it down if you like but you’re most unlikely to succeed.”
The expert’s comments spurred the family to keep trying to find an independent opinion, this time in Australia. After six to eight rejections, they found a Sydney emergency specialist who’d do the job —at $A400 an hour, and he couldn’t start for two months. During this period, however, the reports of Reynolds and ACC arrived — both finding Zac’s treatment was delayed by up to two hours, and that doctors should have considered sepsis earlier.
Reynolds said there were grounds for activating a “code red” referral to critical care as early as 4pm, and regular blood pressure recording might have indicated this threshold had been reached even before 3pm. “In such an event, the emergency medical team would have been called and it is highly likely that Zachary would have received more intensive care two or even three hours earlier than eventuated.” For meningococcal patients, said ACC’s expert, Andrew Munro, a specialist from Nelson Hospital, every untreated hour in the emergency department increases the risk of death by up to 13 per cent.
Lance Gravatt says his son would be ashamed of the treatment he was given — and how the medical community had dealt with the family since. Zac had wanted to be a doctor from the time he was little — he’d even dress up as one — and had to overcome dyslexia to achieve top grades at Auckland Grammar.
But it was his father’s serious illness in 2004 — when Lance was hospitalised nine times for seven bowel operations — that ultimately decided him. “He said he could remember standing at the end of my bed looking at me and feeling totally helpless and he decided he never wanted to feel like that again. But the irony is that’s exactly what happened to Zac. We all just stood by helplessly and watched him die.”
He says when the family arrived back from Wellington just before 5pm the day Zac died, they saw him only briefly before he was rushed to critical care. He was in severe pain and barely able to talk. “The last thing he said to me was to ask who was here. I said, ‘We’re all here, Mum, Maddy and me.’ “He said, ‘I suppose Mum’s freaking out,’ and I said, ‘No, she’s not.’ So he’s lying there dying and he’s thinking of Mum.”
Lance says the family had no idea how critical Zac’s condition had become, re-assured by the consultant’s calm manner. “But then I heard someone say, ‘We’ll just have to bag him and run’ [a reference to the respiratory bag] and I thought, ‘That doesn’t sound good.'”
Says Jenny: “They said I might like to go up with Zac in the lift — ‘We’ll let you know.’ But they didn’t. I just saw this vision of six people around his bed pushing him with someone on the bag just going hell for leather.” They also thought it was odd that they were asked to wait in the critical-care department’s whanau room, rather than being taken to see him. Lance recalls phoning a friend to get a priest.
“I still thought Zac was going to live but I had this intuition this wasn’t going well.” Those fears were heightened when a critical-care nurse arrived and told them staff were “doing everything they can for him”.
“You’ve watched enough of those medical movies to know that isn’t good. She was still talking to us when another nurse rushed in and said: `If you want to see Zac before he dies, you’d better run now.’ “They put us in the room next to Zac. There was a big window with a blind and they just lifted the blind and it was the worst thing I’ve ever seen.”
Zac, grotesquely swollen and covered in the meningococcal rash, was already dead.
Tests at post-mortem showed that Zac Gravatt died of meningococcal C — a strain of the disease that Environmental Science and Research (ESR) told the Gravatts almost certainly came from someone who had recently arrived from overseas.
Lance believes it was most likely carried by one of the swine-flu patients Zac had seen on the wards the previous week.
Zac had been vaccinated against meningococcal B at school, but hadn’t been offered any further shots despite Australasian emergency medicine policy saying all health-care personnel should be offered vaccinations against any vaccine-preventable disease. A vaccine is available for meningococcal C and, in Lance’s view, that’s just one more failing by the DHB.
He says the board’s new chief medical officer, Margaret Wilsher, who started the job in July, has “picked up the issues and made things happen”, so he is now more confident they will reach some reconciliation. The board has apologised to the Gravatt family for the shortcomings in Zac’s care. Wilsher told Metro that while it doesn’t know whether earlier treatment might have saved him, “we missed an opportunity”.
The eight-week swine-flu epidemic had swamped the hospital. “Almost all hospitals crumbled to some degree.” Although a registrar had first logged into Zac’s case just four minutes after he arrived in the adult planning unit (APU) from the emergency department, it was likely he was interrupted, possibly many times, before he completed his assessment more than 100 minutes later.
Wilsher says the board “totally accepts” the findings of the Reynolds report, and also regrets failures in the hospital’s cornmunication after Zac died. “It’s apparent that once Zac had died, it was as though the care of the hospital stopped.”
New systems have been instituted to try to prevent a similar tragedy. The hospital has appointed three more senior doctors to support the general medical services in the emergency department and APU. Patients assessed at triage as in category 3 (as Zac was) or 4 (less serious) are now automatically reassessed immediately on arrival in the admitting ward.
The board has also developed a scoring tool to allow patients who are physiologically unstable, as Zac was, to be recognised earlier. It was trialled on cardiac patients and is due to be introduced before the end of the year.
The board is also re-examining criteria for which cases are investigated internally at formal morbidity and mortality reviews. While Zac’s death at the time was “certainly shocking”, says Wilsher, it was not considered surprising in terms of presentation and the rapid progression of meningococcal disease, which itself could be very difficult to recognise.
“We should be reviewing a lot more of our deaths in hospital because if you scratch below the surface you may find elements of the care that were not done at all as well as one might think.”
Lance Gravatt points out, however, that the board promised former health commissioner Ron Paterson after a similar case to Zac’s two years earlier, in 2007, that an early-warning scoring system would be established then — but it was not. “How many innocent people have got to die before the DHBs actually make good the undertakings they make — and who fol¬lows it up? What sort of system have we got when years go by and nothing is done?”
He says it shouldn’t be up to ordinary Kiwis to have to police the system. “The legislation has largely stripped us of any rights to sue. The system is meant to be quick, cheap and accessible. It’s turned out very expensive for us, very inaccess¬ible and it doesn’t bloody work.”
While Wilsher had apologised “ex officio”, it still rankled that not one of the doctors or nurses involved in Zac’s care that July day had done so. “In New Zealand, all you ever get is an apology. I just feel like not only have you got to batter Fortress Medicine down to get a review, having battered it down you can’t even get the people involved to say, `I’m sorry.” Wilsher told Metro that apologies for members of the medical team “are a very personal matter. The apology must come from me. As the most senior member of the clinical team, I am accountable for the care.”
Auckland Medical School professor of general practice Bruce Arroll, with whom Zac worked as a summer student last year, says he is appalled at the closed shop the Gravatts encountered when they tried to get an independent opinion from the wider medical community.
“I think doctors probably need to change their mindset. We just don’t like criticising each other, and that’s unfortunate. We have to become more critical of each other. People didn’t want to think something terrible had gone wrong — they wanted to believe nothing had. There was self-delusion.”
Lance Gravatt says he told the DHB that simply “re-educating people” doesn’t cut it. “That’s like reminding people to do their job. Some really organic things have to change to make it better. This is the final legacy that Zac can leave medicine — to make it better.”